Neuropsychiatry is a medical discipline that integrates the principles of neurology and psychiatry to manage mental health conditions with neurological origins. This specialty emphasizes the intricate relationship between brain function and behaviour, addressing disorders arising from brain injuries, dementia, or other neurological diseases. Neuropsychiatrists apply their dual expertise to diagnose and treat psychiatric symptoms linked to or resulting from nervous system dysfunctions.

Functional Neurological Disorder (FND) is a condition where the brain sends and receives signals incorrectly. It is often described using a "Computer Analogy."
"In FND, the hardware of the brain (the structures, nerves, and wires) is healthy and intact, but there is a problem with the software (the way the brain processes and sends information)."
FND is no longer a "diagnosis of exclusion" (only diagnosed when everything else is ruled out). Instead, specialists look for positive clinical signs that are unique to FND.
Limb weakness, paralysis, tremors, or "functional" tics.
Episodes resembling epilepsy but without abnormal electrical brain activity.
Numbness, tingling, or "vision tunnels" that don't follow nerve paths.
"Brain fog," sudden memory gaps, or difficulty word-finding.
A neurologist or neuropsychiatrist identifies FND through specific tests, such as:
Because FND sits at the intersection of mind and body, the most successful treatment involves a Multidisciplinary Team (MDT).
Neuropsychiatrists are uniquely trained to manage the "Why" and the "How" of FND. They treat the neurological symptoms while simultaneously addressing the psychological drivers—such as past trauma, high-stress environments, or maladaptive coping mechanisms—that may be fueling the brain's "software" errors.
Modern research has moved away from seeing FND as a purely "psychological" problem. As of 2025–2026, the scientific consensus describes FND as a disorder of brain network connectivity and predictive processing.
The brain is no longer viewed as a passive receiver of information, but as a "prediction machine" that has developed a glitch in its expectations.
Latest neuroimaging (fMRI) shows that in FND, specific brain networks are "talking" to each other too much or too little.
This is currently the leading theoretical model for FND (supported by the latest 2025 Wartenberg Lecture and research by Prof. Jon Stone and others).
Research in 2024–2025 has clarified why some people develop these faulty circuits while others don't. It is rarely one single cause, but a "perfect storm"
Childhood adversity or genetic "startle" sensitivity.
Sensitizes the Amygdala, making the brain more reactive to threat.
A physical injury, a bad migraine, or an acute panic attack.
Acts as the "trigger" that creates the first software glitch.
Anxiety about the symptoms, social isolation, or lack of diagnosis.
Reinforces the faulty Predictive Coding loop, making symptoms stick.
FND is the result of a brain that has become hyper-focused on its own internal predictions and has disconnected its emotional centres from its voluntary control centres.
The "hardware" is fine, but the integration of different brain regions is misaligned. This is why treatment involves "multimodal" therapy—you have to retrain the motor circuits while simultaneously calming the salience and limbic (emotional) circuits.
In the field of neuropsychiatry, "missed diagnosis" refers to two distinct risks: failing to identify FND in a patient (leading to unnecessary treatments) or incorrectly labelling a structural disease as FND (leading to delayed life-saving care).
Modern research indicates that the historical fear of a massive "misdiagnosis epidemic" is outdated, but the stakes for the individual remain high.
Misdiagnosis in this field typically occurs in one of two directions. Research shows that both directions occur at a similar rate - approximately 4% to 5%.
This occurs when a structural neurological condition is mistakenly diagnosed as FND.
This occurs when a patient’s functional symptoms are treated as structural damage.
When an FND diagnosis takes years to confirm (the current average is often years), several secondary risks emerge:
Muscle Atrophy: Disuse of a "functional" limb can lead to actual muscle wasting or joint contractures.
Medical Gaslighting: Patients feel disbelieved, leading to "diagnostic trauma" and a breakdown in trust with the medical system.
Economic Drain: Studies show FND patients have higher healthcare costs before diagnosis due to repeated ER visits and unnecessary MRIs.
"Hard-Wired" Symptoms: The longer a faulty circuit is used, the harder it becomes to "retrain" via neuroplasticity.
Neuropsychiatrists now use the "Diagnosis of Inclusion" strategy to minimize these risks:
Research Fact: A systematic review by Stone et al. found that since 1970, the rate of misdiagnosis for FND has dropped significantly due to better imaging, yet the stigma of the diagnosis remains the biggest barrier to early treatment.
Functional Neurological Disorder (FND) can feel like being handed a complex manual written in a language you don’t quite speak yet. Because FND sits right at the intersection of neurology and psychiatry, your care plan needs to be equally "bilingual."
Here is a care-coordination checklist designed to help you navigate the first few months of treatment and ensure no part of your recovery is overlooked.
Phase 1: Confirmation and Education
The first step in "retraining the brain" is fully believing and understanding the diagnosis. Doubt acts like noise that interferes with the retraining process.
Phase 2: Assembling Your Multidisciplinary Team (MDT)
FND is rarely treated by a single doctor. It takes a village—specifically, a neurological one.
Phase 3: Immediate Management Strategies
While waiting for therapy appointments, these "first aid" steps can help manage daily symptoms.
Based on the world-leading FND resource Neurosymptoms.org (created by Professor Jon Stone), Functional Neurological Disorder symptoms are categorized into "Core FND Symptoms" and "Common Associated Symptoms."
These are the primary symptoms that define the disorder, often described as "software" glitches where the brain's signals are blocked or distorted.
Neurosymptoms.org emphasizes that while these are not "defined" as FND, they are incredibly common in FND patients and are often part of the same underlying "circuitry" issue.
1. Hoover’s Sign (For Leg Weakness)
This is perhaps the most famous test for functional limb weakness.
2. The Entrainment Test (For Tremors)
This test looks at whether a tremor is "fixed" by brain structure or "fluid" based on brain attention.
3. Tubular Vision (For Visual Symptoms)
In structural vision loss, the visual field expands the further away you get from an object.
4. Hip Abductor Sign
Similar to Hoover’s sign, this test involves the patient pushing their legs outward.
5. Signature Signs of Functional Seizures
Unlike epileptic seizures, functional seizures often have specific "positive" markers:
Neuro-physiotherapy
Bypasses the "broken" conscious pathway to use automatic ones.
Cognitive Therapy
Addresses the "noise" (stress/anxiety) that jams the signals.
Occupational Therapy
Provides tools to navigate the world while the brain heals.
A Quick Reminder: Recovery in FND is rarely a straight line. It’s often "two steps forward, one step back," and that’s perfectly normal for a brain that's learning to reboot its software.
FND isn't just about recording what went wrong; it’s about finding patterns. Because FND is a "software" issue, your brain often reacts to hidden triggers like fatigue, sensory overload, or even "emotional echoes" from earlier in the day. This tracker is designed to help you and your neuropsychiatrist identify those glitches.
How to use this: Don't just list the symptom; list what was happening around it. Look for the "Pre-Symptom" state.
Cognitive Therapy
7
Walking in a loud mall
High stress, 5hrs sleep
Sat down, listened to music
At the end of each day, give yourself a quick score (1-5) on these three areas. Over time, you’ll likely see that when these scores are low, symptoms are high.
FND recovery can feel slow. It is vital to track functional wins, no matter how small.
Neuroplasticity Tip: When you record a "win," you are actually reinforcing the healthy neural pathways in your brain. You’re telling your "software" that it’s doing a good job.
When you go to your next appointment, don't just say "I'm having a hard time." Show them the tracker and say:
"I noticed my symptoms spike on Tuesdays after my loudest meeting, or whenever I get less than 6 hours of sleep. How can we adjust my 'Pacing Plan' to account for this?"
In the context of FND, grounding isn't just about "calming down"—it is a neurological tool used to redirect the brain's attention away from malfunctioning internal signals and back to the external environment. This helps "reset" the software glitch.
Here is a list of grounding techniques specifically categorized for FND management.
1. Sensory "Jolts" (To Break a Symptom Cycle)
These are high-intensity sensations designed to grab the brain's attention immediately. They are particularly useful for functional seizures or sudden paralysis.
2. Cognitive Distraction (The "Software Override")
FND symptoms often worsen when the brain "focuses" on them. These techniques force the brain to use its processing power elsewhere.
3. Physical "Automaticity"(For Motor Symptoms)
These techniques help the brain bypass "conscious" movement and return to "automatic" movement.
4. The "5-4-3-2-1" Method (TheGold Standard)
This is the classic grounding exercise, adapted for FND by focusing on externalizing your awareness
Grounding is a skill, like a muscle.
The secret is "Movement without Thinking." Since the "positive signs" proved that your muscles can work when the brain is distracted, these goals focus on tricking the brain into using those automatic pathways again.
Goal 1 : Utilizing the Hoover’s Sign Mechanism
Goal 2 : Breaking the Tremor Rhythm (Entrainment)
Goal 3 : Restoring Gait (Walking) via "Glitches"
One of the biggest hurdles in FND rehab is overdoing it on a "good" day, which leads to a massive symptom flare-up the next day.
Ensure your Physical Therapist (PT) and Neuropsychiatrist are aligned on these goals. Your PT focuses on the movement, while your Neuropsychiatrist helps manage the fatigue and anxiety that might be making the "software" glitch more frequently.
A brain injury—whether caused by a sudden trauma (Traumatic Brain Injury) or a medical event like a stroke or hypoxia (Acquired Brain Injury) — is never just a physical wound. It is a fundamental shift in how a person thinks, feels, and interacts with the world. Neuropsychiatry focuses on managing the "invisible" symptoms that often persist long after the physical scars have healed.

Brain injuries often affect specific "hubs" that regulate our personality and emotional control. The most commonly affected areas include the Frontal Lobes (the CEO of the brain) and the Temporal Lobes (the memory and emotion centre).
When these areas are damaged, the "brakes" of the brain are often removed, leading to:
The aftermath of a brain injury often involves a "constellation" of psychiatric symptoms that require specialized management.
Depression, Mania, Apathy
Occurs in up to 50% of patients in the first year post-injury.
PTSD, Generalized Anxiety, Panic
Often linked to the circumstances of the injury (e.g., a car accident).
Delusions, Hallucinations
Less common, but can occur with severe temporal lobe damage.
Irritability, "TBI Rage"
Often triggered by overstimulation or cognitive fatigue.
One of the most misunderstood aspects of brain injury is neuro-fatigue. Unlike normal tiredness, this is a profound exhaustion of the brain's processing power.
The Battery Analogy: A healthy brain starts the day with a 100% charge and uses 1% for a conversation. A brain-injured person may start at 50% and use 40% just to process the background noise of a busy grocery store.
Neuropsychiatric care for brain injury is not about "curing" the injury, but about maximizing function and quality of life.
Recovery from a brain injury is a marathon, not a sprint. A neuropsychiatric evaluation provides the roadmap for navigating the cognitive and emotional hurdles of that journey.
This checklist is designed to help families and caregivers bridge the gap between daily observations and clinical appointments. Tracking these changes helps your medical team fine-tune medications and therapy strategies.
Use this list to note the frequency and severity of symptoms over the past 2–4 weeks.
These symptoms are often the result of damage to the limbic system or frontal circuits.
Documenting these helps the neuropsychiatrist understand the "cognitive load" the patient can handle.
These often act as "fuel" for psychiatric symptoms.
When you observe a specific behavioural incident (like an outburst), try to record it using this framework:
What happened right before?
"We were in a loud restaurant for 30 minutes."
What exactly did they do?
"Shouted at the waiter and began to cry."
What helped them calm down?
"Going to the quiet car and sitting in silence."
Pro Tip: If possible, keep a brief "Sleep and Mood" log for one week prior to the appointment. Often, a spike in behavioural issues correlates directly with a poor night's sleep.
Creating a "brain-friendly" environment is one of the most effective ways to reduce irritability and prevent neuro-fatigue. By lowering the amount of raw data the brain has to process, you preserve the patient’s limited mental energy for more important tasks, like rehabilitation and social connection.
Reducing Cognitive Load at Home
The brain uses a massive amount of energy to process visual information. Flickering lights or cluttered rooms can lead to "visual noise" that triggers headaches and irritability.
For someone with a brain injury, background noise isn't just a distraction—it's physically painful and exhausting.
Since the brain’s internal filing system is often damaged, we move that system to the physical environment.
Fluorescent, bright, flickering.
Soft, indirect, warm-toned.
Open shelves with many colors/labels.
Items behind closed cabinet doors.
Hardwood or tile (loud, echoing).
Rugs or carpets (muffled sound).
Spontaneous, "play it by ear."
Predictable, written on a wall calendar.
Every home should have a designated "Quiet Zone" or "Low-Stimulation Pod." This is a corner or room where:
1. There are no screens or electronics.
2. Conversations are not allowed.
3. The lighting is very low.
4. Comfortable seating (like a beanbag or recliner) is available.
Encourage the patient to go here before they feel overwhelmed. Once a "meltdown" starts, it's often too late for the Quiet Zone to be fully effective.
Neuropsychiatry is a growing subspeciality under Medicine. Over the past century there has been a greater awareness in the dimensions of the Brain and Mind. Such exploration has bought new hopes to individuals struggling with complex disorders in the interactions between the brain and mind.
As the Brain and mind components are so closely wired together, any disruption to mutual circuits due to an injury or inflammation would result in disease of the mind. This would present with disturbance in mood, sleep, energy levels, motivation, memory and thinking. This is a Neuropsychiatry disorder and can be treated. If you have been diagnosed with a Neurological or Neurosurgical condition and your doctor or you believe you have comorbid mental health impact, you are best to consult a Neuropsychiatrist.
Traditionally these conditions would be managed by Psychiatrists, Neurologists and other neuroscience specialists. Such expectation has been lost in the vast array of expansion within their own fields.
Neuropsychiatrist uniquely get trained in this space allowing a better focussed approach to management and holistic treatment of such conditions. Today, we have new optimism to these conditions with greater scope of recovery especially when diagnosed and treated early.
A Neuropsychiatrist has a wide range of training. The bulk of the specialist’s time is spend within the Neuroscience space looking and studying brain images, examining key neurological signs and utilising specialised cognitive and bio marker tests to reach diagnostic conclusions. Yet, the primary strength of their work is in the understanding of complex psychiatric, neurological process and its interplay.
The neuropsychiatry of movement disorders is a specialized field focusing on the complex intersection of motor control, emotion, and cognition. While movement disorders like Parkinson’s or Huntington’s are often defined by physical symptoms (tremors or stiffness), they are deeply intertwined with psychiatric conditions such as depression, anxiety, and behavioural changes.
At the heart of this field lies the basal ganglia, a group of subcortical nuclei responsible for "gatekeeping" both our movements and our moods. When these circuits are disrupted, the result is often a dual challenge: motor dysfunction and neuropsychiatric distress.
The primary neurotransmitter involved is dopamine. In neuropsychiatry, we often look at the "Goldilocks" principle of dopamine:
Neuropsychiatric consequences of Parkinson's disease can include depression, anxiety, psychosis, apathy, and impulse control disorders. These symptoms can impact a person's quality of life and make it harder to treat the physical symptoms of Parkinson's.
Historically, the psychiatric symptoms of these disorders were treated as "secondary" or "reactions" to the physical disability. Modern neuropsychiatry views them as primary biological symptoms caused by the same brain pathology affecting movement.
Clinical Insight: A patient with Parkinson’s may experience "off-period" anxiety, where their mood plummets exactly when their motor medication wears off. This proves that the motor and emotional circuits are physically linked.
Managing these conditions requires a multidisciplinary "whole-person" approach:
This list is designed to help you and your care team look "under the hood" of Parkinson’s Disease. Often, neurologists focus on your gait and tremor because those are easy to see. These questions ensure the non-motor symptoms get the attention they deserve.
Take these questions to your next appointment. It can be helpful to have a family member or close friend answer them with you, as they may notice subtle shifts in your behaviour before you do.
1. Mood and Motivation
2. Thinking and Memory (Cognition)
3. Behaviour and Impulse Control
This is especially important if you are taking Dopamine Agonists (like Pramipexole or Ropinirole).
4. Sleep and Perception
Track your mood specifically during times when your motor symptoms are at their worst.
A spouse or child can report behavioural changes like irritability that the patient might not perceive.
Pick the top two non-motor symptoms that bother you most. Don't try to solve all of them in one visit.
A Note on Candor: Don't be embarrassed to mention things like hypersexuality or gambling urges. These are medical side effects, not moral failings. Your doctor needs to know so they can adjust your "dopamine budget."
Managing Parkinson’s disease (PD) alongside mental health conditions like depression or anxiety is a delicate balancing act. Because PD medications increase dopamine and many psychiatric drugs affect serotonin or block dopamine, they can sometimes "clash."
This guide summarizes the key interactions you should discuss with your neuropsychiatrist or neurologist.
These combinations require careful monitoring by a specialist.
(e.g., Selegiline, Rasagiline)
SSRIs/SNRIs (e.g., Prozac, Zoloft, Effexor)
Serotonin Syndrome: A rare but serious condition of "serotonin overload" causing confusion, high fever, and muscle rigidity.
(Sinemet)
Typical Antipsychotics (e.g., Haloperidol, Risperidone)
Dopamine Blockade: These psychiatric meds "cancel out" your PD meds, potentially causing a severe worsening of tremors and stiffness.
(Apokyn)
Ondansetron (Zofran)
Severe Hypotension: Can lead to a dangerous drop in blood pressure or loss of consciousness.
These medications are generally preferred because they have a lower risk of interfering with your motor control.
When we treat Parkinson's, we are trying to fill a "dopamine tank" that has a leak.
Important Note on Impulse Control: If you are taking a Dopamine Agonist (like Pramipexole or Ropinirole), adding certain antidepressants can occasionally change how your brain processes "rewards." If you notice a sudden urge to gamble, shop excessively, or eat uncontrollably, tell your doctor immediately. This is a chemical side effect, not a lack of willpower.
While rare, it is vital to know the difference between a reaction to too much serotonin and a reaction to stopping dopamine.
Too much serotonin (often MAO-B + SSRI).
Fast heart rate, shivering, sweating, hyper-reflexes (twitchy).
Sudden stop of PD meds or starting heavy dopamine blockers.
Extreme muscle "lead-pipe" rigidity, very high fever, mental confusion.
Managing these medications is a team effort. Never stop a psychiatric or PD medication "cold turkey," as this can trigger a medical emergency.
Caring for the Mind While Supporting the Body
When a loved one has Parkinson’s, you aren't just managing appointments and medications—you are often navigating a profound shift in their personality and your relationship. This guide is designed to help you stay grounded when the "invisible" symptoms become overwhelming.
It is normal to feel a sense of grief, even though your loved one is still here. Neuropsychiatric symptoms like apathy or personality changes can make you feel like the person you knew has slipped away.
When cognitive "fog" or irritability sets in, standard communication often fails. Try the Three-S approach:
Loss of dopamine in the "reward" centre.
Don't ask, just do. Instead of "Do you want to walk?", say "It's time for our 5-minute walk," and hand them their shoes.
Chemical imbalance or med side effects.
Validate the emotion, not the vision. "I don't see the person in the corner, but I can see that it's making you feel scared. Let's go into the kitchen."
"Thin" emotional brakes.
The 10-foot Rule. If they are escalating, physically move 10 feet away. Reducing your physical "presence" can lower their sensory input and de-escalate the situation.
You cannot pour from an empty cup. Caregiver burnout isn't just "tiredness"; it's a physiological state that mirrors the patient's own stress.
A Final Thought: You are the most important part of your loved one's treatment plan. By protecting your own mental health, you are providing them with the stable, calm environment their brain needs to function at its best.
Understanding the "Triad" of Symptoms
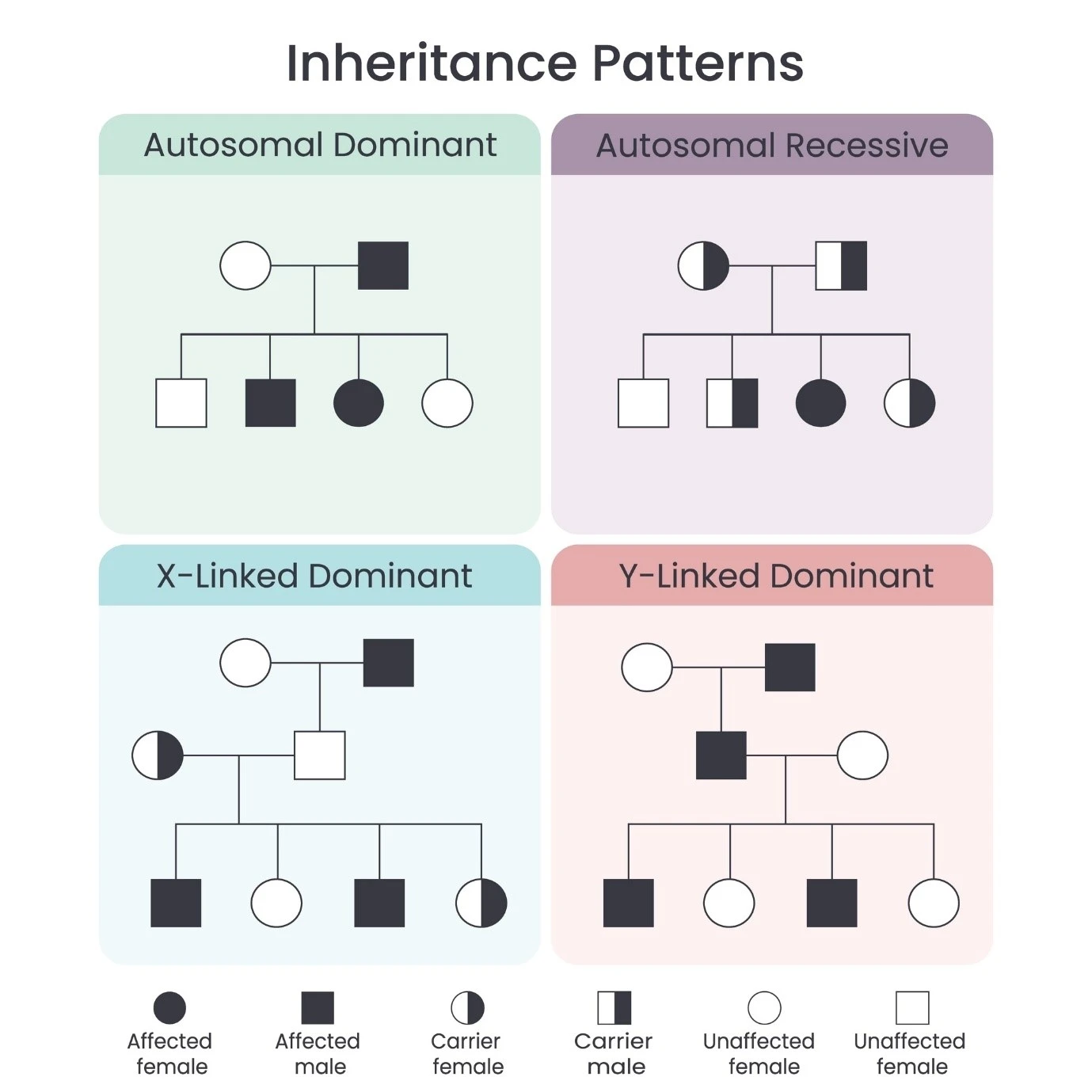
Huntington’s Disease (HD) is a unique and challenging genetic condition. Unlike many other neurological disorders, HD is defined by a "Triad" of symptoms: Motor, Cognitive, and Psychiatric. While the "chorea" (involuntary dancing movements) is the most visible sign, the neuropsychiatric symptoms often appear years earlier and can be the most distressing for both the individual and their family.
The Biological Root: The Striatum
HD is caused by a genetic mutation that leads to the progressive breakdown of nerve cells in the brain, particularly in the striatum (part of the basal ganglia). The striatum acts as the brain's "volume knob" for both movement and emotion.
When the striatum atrophies, the "brakes" on behaviour and movement are released. This leads to the characteristic physical movements and the "disinhibited" or impulsive behaviours seen in neuropsychiatry.
The Huntington’s Triad
Chorea (twisting), rigidity, slurred speech.
Can lead to social withdrawal and "movement anxiety."
Difficulty planning, "getting stuck" on ideas.
Known as "executive dysfunction"; causes frustration.
Irritability, apathy, depression, OCD.
Often the most disabling part of the disease for families.
This is often the most difficult symptom for caregivers. It isn't "anger" in the traditional sense; it is a biological inability to regulate frustration.
Apathy is the most common psychiatric symptom in HD. The person may sit for hours and show no interest in hobbies they once loved.
A person with HD may ask the same question repeatedly or become obsessed with a specific idea (e.g., wanting to go to the store now). This is a result of the brain's "switching" mechanism being damaged.
Because HD is a "family disease," the treatment must be multidisciplinary.
The Neuropsychiatrist's Role: In HD, the goal is to "smooth out" the emotional peaks and valleys. By stabilizing the psychiatric symptoms, we allow the person to remain engaged with their family for as long as possible.
This requires a shift from "persuading" to "facilitating." Because the brain’s "switching" and "filtering" mechanisms are physically damaged, traditional arguments or logic often fail.
This toolkit provides actionable strategies to handle the two most challenging behavioural symptoms: Perseveration and Irritability.
Perseveration happens when the brain gets stuck on a loop—a single question, a specific task, or a perceived need. It is not "stubbornness"; it is a failure of the brain's internal gear-shifter.
Irritability in HD is often a "thunderstorm" in the brain caused by sensory overload or a sudden change in plans. The "brakes" that normally stop an angry impulse are simply no longer there.
Use this table as a quick reference for daily interactions.
"Stop asking me that!"
"I wrote the answer on the fridge."
Uses visual cues to bypass damaged memory circuits.
"Hurry up and choose."
"Take your time. I'll check back in a minute."
Respects the processing delay (bradyphrenia) common in HD.
"We're going to the store, then the bank, then lunch."
"We are going to the store now."
Prevents cognitive "bottlenecking" and overwhelm.
Detailed explanations.
Short, 5-word sentences.
Keeps the "mental load" low and manageable.
Predictability is the best "medication" for HD irritability. When the brain knows what is coming next, it doesn't have to work as hard to process the world.
Consistent communication can significantly lower the need for sedative medications.
This plan is a vital document for any household or care setting dealing with Huntington’s Disease (HD). Because "HD Rage" is a biological event—akin to a seizure of the emotional centers—traditional "parenting" or "policing" techniques will fail. This protocol focuses on safety, de-escalation, and dignity.
A Guide for Family, Friends, and Visiting Staff
Before a full outburst, there is usually a buildup of internal pressure.
At this stage, the frontal lobe (the logic center) has essentially "gone offline." The person is in a fight-or-flight state.
The Safety Protocol:
After the adrenaline drops, the person with HD will often feel profound exhaustion, confusion, or even shame.
Share this table with any new healthcare worker or guest.
Give 6ft of personal space.
Prevents sensory "crowding."
Keep hands visible and still.
Unexpected touch can trigger a "startle" rage.
Agree or distract.
Logic is not accessible during an HD event.
Look at the floor or a neutral object.
Reduces the "threat" response in the amygdala.
If the person becomes a danger to themselves or others, or if a weapon is involved, it is a medical emergency. Contact emergency services or the local AE mental health team.
Epilepsy is more than a tendency to have recurrent seizures; it is a complex neurological condition that frequently involves psychiatric symptoms. The field of neuropsychiatry focuses on understanding how these seizures, the underlying brain dysfunction, and the treatments used affect a person's mood, cognition, and behaviour.

Neuropsychiatric consequences of epilepsy can include a range of mental health issues often arising from the direct impact of seizures on the brain, the social stigma associated with epilepsy, and potential side effects of anti-seizure medications; with a complex bidirectional relationship where epilepsy can trigger psychiatric symptoms and pre-existing mental health conditions can exacerbate seizure activity.
Psychiatric disorders are significantly more common in people with epilepsy (PWE) than in the general population. This is often due to shared biological pathways rather than just a reaction to having a chronic illness.
~30% - 50%
Often presents as "interictal dysphoric disorder" (irritability, insomnia, and mood swings).
Anxiety ~20% - 25%
Can include generalized anxiety, panic attacks, or fear related to seizure occurrence.
~2% - 7%
May occur after a cluster of seizures (postictal) or independently (interictal).
High in Children
Often linked to frontal lobe dysfunction or the side effects of medications.
In neuropsychiatry, we categorize symptoms based on when they occur in relation to a seizure. This helps doctors determine the best treatment path.
The relationship between epilepsy and psychiatry is bidirectional. This means that people with depression are more likely to develop epilepsy, and vice versa.
The Limbic System (including the hippocampus and amygdala) plays a dual role: it is the most common site for focal seizures (Temporal Lobe Epilepsy) and the primary center for emotional regulation. When these circuits are disrupted by electrical "storms," both movement and mood are affected.
Key biological factors include:
Managing neuropsychiatric symptoms in epilepsy requires a delicate balance. A multidisciplinary approach is essential.
Some Antiseizure Medications (ASMs) can impact mood:
Because of the stigma often associated with both epilepsy and mental health, therapy (CBT) and support groups are vital for improving the quality of life.
Important Note: Stopping or changing seizure medications without medical supervision can lead to status epilepticus (prolonged seizures) or a rebound in psychiatric symptoms. Always consult your neurologist and neuropsychiatrist before making changes.
Selecting an antiseizure medication (ASM) often involves a "buy one, get one" approach: a drug might help control your seizures while also treating a mood disorder, or it might unfortunately worsen it.
Here is a detailed breakdown of how common medications can influence your neuropsychiatric health.
The effects of these medications can generally be categorized into positive (psychotropic/stabilizing), negative (depressant/irritating), or mixed.
Lamictal
Often acts as an antidepressant. Highly effective for bipolar depression and overall mood stability.
Depakote
A powerful mood stabilizer. Excellent for controlling mania, aggression, and impulsivity.
Keppra
Can cause "Keppra-rage" (extreme irritability, hostility, or agitation) and depression in sensitive users.
Topamax
Known for "cognitive fog": word-finding difficulties, slowed thinking, and increased risk of depression.
Neurontin
Often has anxiolytic (anti-anxiety) effects and can improve sleep quality. But can cause the brain fog.
Fycompa
Carries a "Black Box" warning for serious behavioral changes, including aggression and suicidal ideation.
Tegretol
Used to treat mania and can help stabilize mood, similar to valproate.
Luminal
High risk of depression, lethargy, and hyperactivity (paradoxical) in children.
These are two of the most common patient-reported side effects in the epilepsy community:
In rare cases, a patient’s seizures are finally brought under control (the "normalization" of the EEG), but as the seizures disappear, psychiatric symptoms like psychosis or severe anxiety suddenly emerge. It is as if the brain used the seizure activity to "vent" electrical energy, and stopping them creates a different kind of pressure.
Most psychiatric side effects are dose-dependent. Starting at a very low dose and increasing it slowly (titration) allows the brain to adapt, significantly reducing the risk of a negative mood reaction.
Pro-Tip: If you have a personal or family history of depression or anxiety, mention this to your neurologist. They may choose a "mood-positive" medication like Lamotrigine to support your mental health while treating the epilepsy.
Tracking the relationship between your seizures and your mood is one of the most powerful things you can do for your care team. Since memory can be a bit "foggy" (especially after a seizure or on certain meds), having a paper or digital trail turns "I think I’ve been moody" into "I’ve had 4 days of high irritability following my last seizure."
Here is a structured template you can print or copy into a notes app.
Focal (2 min)
3/10
High irritability (Rage)
Missed morning dose; poor sleep.
When filling out the "Primary Mood Symptom" column, look for these common neuropsychiatric markers:
A Note on Safety: If you track a mood score of 1 or 2, or experience thoughts of self-harm, do not wait for your next appointment. Contact your neurologist or neuropsychiatrist immediately.
When you head into your next appointment with your data in hand, you want to move the conversation from "I feel bad" to "How do we fix this clinically?"
Here is a list of targeted questions categorized by the specific issues you might be seeing in your tracker.
If your mood shifts seem to "orbit" your seizures:
If your main struggle is thinking clearly
Doctors are often short on time. Start with: "I've been using a mood tracker, and I've found a consistent pattern of [X] happening [Y] days after my seizures. I'd like to review my medication's role in this."
The field of neuropsychiatry in epilepsy has shifted rapidly in the last 24 months (2024–2026). The focus has moved from merely "managing side effects" to precision neuropsychiatry, where we use specific medications to treat both the seizures and the underlying brain network dysfunction simultaneously.
Here is a summary of the most recent evidence and clinical shifts as of 2026:
The most significant breakthrough in 2025–2026 is the clinical trial data for XEN1101 (a potassium channel opener).
Recent real-world data (late 2025) has provided a surprising update on Cenobamate, one of the most powerful new drugs for focal seizures.
Validated in 2025, the Seizure Related Impact Assessment Scale (SERIAS) has become the "gold standard" for neuropsychiatric tracking.
There is mounting evidence (2025-2026) linking chronic neuro-inflammation to the "psychosis of epilepsy" and "forced normalization."
The International League Against Epilepsy (ILAE) updated the seizure classification system in 2025.

At “All Psychiatry” our team of Australian- certified mental health clinicians provides expert care tailored to your needs.
We have made it simple and efficient - just follow the steps below to get started

To get started, please obtain a referral from your GP addressed to “All Psychiatry” and include as much information as possible.
It helps to include information about your symptoms, history and any previous treatment.
You can upload your referral securely on our website, or ask your GP to fax it to 03 8080 6484 or email it to admin@allpsychiatry.com.au
Once our friendly admin team receives your referral, it will be promptly reviewed to match you with the specialist best suited to your needs. Someone from our admin team will contact you to arrange your appointment
Neuropsychiatry bridges the gap between neurology (which focuses on the brain’s physical disorders) and psychiatry (which deals with mental health conditions). It examines how brain disorders impact mental health and behavior.
You might need a neuropsychiatric evaluation if you experience:
- Memory problems or confusion
- Personality changes
- Unexplained mood swings
- Hallucinations or delusions
- Difficulty concentrating or processing information
- Seizures with mood disturbances
Some conditions can be managed effectively with treatment, but others may require long-term care. The goal is to improve quality of life and symptom management.